Allegro
Crisis and Recovery
Knowledge is Power
Volume CIX, No. 7/8July, 2009
A bargaining history of the Local 802 health fund – what every musician should know
Coping with the cost of health care is a difficult experience for every union in the country. One of the bedrock principles of unions – providing health care for members – is threatened. But at Local 802, this story has a happy ending – for now. Read on to discover how we revived our own health fund from what looked like certain death.
Seven Broadway contract negotiations ago, in 1984, musicians reached a contract settlement with the League that started the Theatre Sick Pay and Hospitalization Fund. It was an important addition to the Broadway contract that, in combination with the Local 802 Health Fund, provided comprehensive health coverage as well as payment if a musician was unable to work due to illness.
Double-digit health care inflation had just started to take hold back then and the Broadway contract called for a contribution to the 802 plan of $20 a week. In 1986 there was more union work in town that included health benefit contributions. It only took $100 in contributions in a six-month period to qualify for Plan A.
The 802 Health Plan built a reserve of money that at one point could continue coverage for plan participants for nearly two years even if employer contributions stopped.
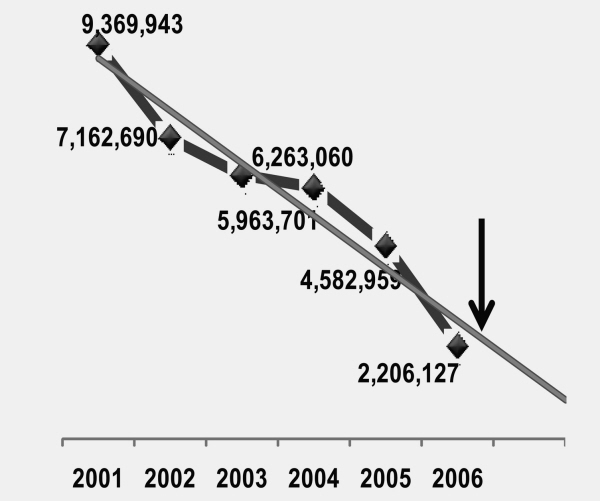 Figure 1. Net assets of Local 802 Health Fund prior to the round of employer increases in 2007. |
MANAGEABLE COSTS
Through much of the 1990’s, health care cost increases were steady but manageable. The Health Fund’s reserves declined but the fund was not threatened. There were several increases in the Plan A contribution level followed by increases in employer contributions.
By 2000, however, costs were spiraling up by double-digit percentages every year. The 802 plan’s reserves dipped below an average year’s claims starting in late 2003. As is illustrated in figure 1, the plan reserves fell by 33 percent from 2001 to 2003.
Fund trustees struggled with the problem. The decline in work meant it was harder for members to achieve the eligibility level. And if that level was increased, even fewer would make the plan. The fund however, needed more resources to pay benefits and the only way was to raise the eligibility level and increase employer contributions.
In 2003 the eligibility level was increased to $1,075 from $975 per six-month period, and employer contribution rates increased in most contracts. On Broadway, musicians saw their contributions rise to $58 per week from $54. This was the first increase since 1994. But that wasn’t enough. The plan was also forced to cut benefits:
- The maximum plan reimbursement was changed from $50,000 per illness to a flat $50,000 per year.
- The in network co-pay was increased to $20, up from $10.
- Changes were made in the prescription drug plan, creating a three-tiered system where generics cost $5, preferred brand name drugs were $30 and non-preferred drugs were $60.
Despite the changes, the net assets of the health benefits plan declined another 65 percent between 2003 and 2006. The national healthcare inflation rate in that period was 43 percent.
In an effort to save money and avoid another eligibility increase or benefit cut, the plan became “self-insured” in 2004.
Instead of buying an insurance policy for its participants, the plan paid the benefits itself, hiring a third party to administer the claims.
Throughout 2005, fund trustees and actuaries held off proposing an eligibility increase, waiting for the “self-insured” savings to materialize. The savings turned out to be over $500,000.
In normal times this might have stabilized the fund. Health care costs however, were continuing to rise at double-digit annual rates and the fund was hemorrhaging money. By the middle of 2006, it was clear the fund was in trouble.
Had the fund trustees – acting on advice from the actuary – imposed an eligibility increase during 2005 and 2006, fewer members would have achieved coverage, but some of the subsequent funding problems could have been moderated. Less would have had to be made up in subsequent negotiations. Figure 2, shows what was lost by not increasing the eligibility rate on Broadway and what the 2007 negotiations had to make up.
By the end of 2006, the 802 plan was close to insolvency. This situation led to drastic changes to the plan that included the following:
- The contribution requirement for plan A coverage increased to $1,300 from $1075 in January 2006 and then to $1,400 at the end of 2006.
- For the first time ever, a participant premium was introduced: $50 per month for individuals and $135 per month for families.
- The cost of generic drugs increased to $20 or 25 percent of the total cost; preferred drugs now cost $40 or 25 percent of the total cost; non-preferred drugs increased to $80 or 25 percent of the total cost.
- The out-of-network deductible rose to $1,000 per person.
FUNDS MERGED
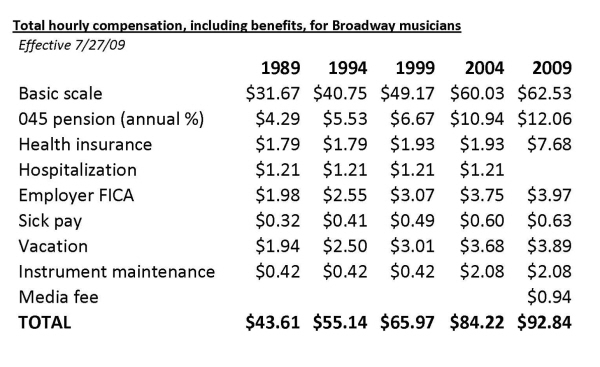 Figure 3. Total hourly compensation, including benefits, for Broadway musicians.. |
During the 2007 Broadway negotiations, the sick pay, hospitalization and 802 health funds were merged. Musicians stepped up and agreed to divert some of their potential wage increases into health care instead. These diversions totaled $88 a week over three years, and in return employers agreed to substantially increase the amount of money contributed to the Health Plan, with the current amount being contributed per chair per week being $218.
Between the merging of the plans and the major increases in employer contributions, 802 was able to create two comprehensive health benefits levels – Plan A+ with hospitalization and Plan A+ without hospitalization. Also, for the first time, subs who do enough work on Broadway – an average of 5.7 shows per week per six month period – will qualify for hospitalization.
These new plans include:
- Restoring the benefits discontinued in 2006 including: the drastic changes for prescription drug coverage, and a 70 percent reimbursement rate for out of network visits.
- Raising the annual cap on benefit payments to $250,000 per year instead of $50,000.
- There are no participant premiums for individuals for either level and the participant premium for family coverage is $200 per month.
The contribution requirement for each six months is $3,200 for medical and $4,300 for A+ with hospitalization. A computation system allows individuals who do an average of 5.7 shows per week on Broadway to qualify for benefits. The reserves of the merged plan were built back up to over six months of claims as of September 2008.
There’s no guarantee for the future, but musicians should know that keeping the Local 802 Health Plan alive and healthy is a big priority for us. The crisis in health care costs affects all of us, and we’re all in it together.
Joel Lefevre, Marisa Friedman, Bill Dennison and Mary Landolfi contributed to this article.