Allegro
‘Just Don’t Kill the Patient’
Member to Member
Volume 116, No. 7July, 2016

The cover of Andrew Schulman’s new book, which is being published this summer by Picador.
The following excerpt is from Local 802 member Andrew Schulman’s new book, “Waking the Spirit: A Musician’s Journey Healing Body, Mind, and Soul,” coming out this summer from Picador. (Read a review here, and info for the book release event here). The story below opens the chapter where Schulman gives an overview of what it’s like to be a resident musician in a surgical intensive care unit.
An attending physician was explaining to a nurse how a new medical device worked while awaiting the arrival of a patient from the operating room. After giving directions for a minute or so he saw that the nurse, a quick learner, would be able to figure out the rest on his own. He turned to walk away and over his shoulder had one last comment, a Parthian shot, delivered with perfect timing:
“Just don’t kill the patient.”
(If you lose your sense of humor in a place like this, it’s time to leave.)
I now had a new adage to add to “soothing and healing” regarding the use of music in the surgical intensive care unit. Just don’t kill the patient.
Joking aside, it’s very important advice, because if music has so much power that it can heal, and even save a life, then certainly it could have the opposite effect.
In August 2011, I was listening to a radio broadcast featuring a doctor who’d been studying the effects of music played during surgery. It was a call-in show and a young physician joined the conversation. He told this story: When he was a medical student, he was on a cardiovascular surgery rotation and assisted during an operation. The surgeon was a fan of heavy metal rock music and played it during the surgery. Very loud. The patient wasn’t doing well and ended up having ventricular fibrillation, went into cardiac arrest, and died.
I couldn’t believe a surgeon would play that kind of music during that kind of an operation. I don’t know if it was the music that killed the patient, but my hunch is that it’s a distinct possibility. At full volume this music could have pushed the patient over the cliff. I was on the edge of the precipice once and the right music pulled me back. I don’t doubt for a second, from what I’ve seen in the past six years, that the opposite could happen. The fact is the patient died, and a very important question is, do you choose the music for the patient’s needs, or the doctor’s?
So – one of the most important decisions you make as a medical musician is choosing what music you play.

Andrew Schulman. Photo: Josh Aronson
Right from the beginning people would ask me what it’s like to be a resident musician in a surgical intensive care unit. By far the question most often asked is, how do you know what to play for patients who are critically ill and not able to say what they’d like to hear? This is the story I always tell to answer that question:
One day shortly after arriving, I was walking past Bed 2. Chris Weist, one of the physician assistants, asked me to play at the patient’s bedside. The woman had a gauze bandage wrapped around the top of her head and appeared to be sleeping. I glanced at her chart. She was in her mid-60s. Chris explained the patient had undergone successful brain surgery the day before and was now heavily sedated. Their main concern was that her blood pressure was high. It hadn’t been below 165 from the time they’d wheeled her in.
Lay-people associate two numbers with blood pressure, as in 120 over 80. The staff in a SICU only refer to the systolic number, the larger number, which measures the pressure in the arteries when the heart beats. The smaller number, the diastolic, measures the pressure between heartbeats when the heart muscle is resting. As in music, it’s the beat that counts.
Different drug therapies had been used but nothing had gotten her lower than 165. Normally, if the systolic number is between 140 and 159 it’s considered high blood pressure, Stage 1 hypertension. But stress can cause spikes in blood pressure and a SICU is by its nature stressful, so concerns only arise if it’s 160 or above and stays that way without medication resolving the issue. As was the case with this patient. Literally from the first day I started, we’d all seen that music had the potential to lower blood pressure. I’d quickly found that playing music with a medium tempo, a beautiful melody, and flowing harmonies – for example, the Gershwins’ “Someone to Watch Over Me” – would in most cases cause the patient to relax. You could actually watch the blood pressure numbers drop within a minute or so, sometimes less. I’d done this hundreds of times already and considered it the easiest thing to do of all the different situations I encountered.
If the patient can’t tell you what they want you search for clues. I looked at her name on the chart and asked her nurse if she knew where the woman was from. She told me the patient’s niece had visited earlier and mentioned the patient was from Puerto Rico.
When I first moved to New York in 1975, one of my neighbors, an actor born and raised in Puerto Rico, had just gotten a grant to do Puerto Rican folklore shows in the city public schools, and he hired me to be his guitarist. There were two beautiful ballads in particular that I’d never forgotten, “Verde Luz” (“Green Light”) and “En Mi Viejo San Juan” (“In My Old San Juan”). I always had the sheet music in one of my folders.
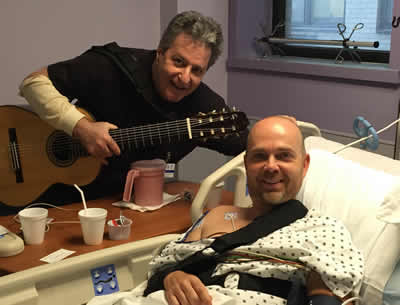
Andrew Schulman uses his music to help hospital patients. Photo: Pilar Baker
I took out the ballads and began to play the entrancing melody of “Verde Luz.” For the first couple of minutes I just looked back and forth at the music and the patient. I didn’t even bother checking the vital signs monitor. This tune was a well-established go-to piece for lowering blood pressure. Finally, I did look up and saw that her blood pressure had indeed changed.
Unfortunately, in the wrong direction.
It was now 168. I wasn’t concerned though because I knew that a person might have a bad association with a particular song – maybe there was a romantic breakup or some other negative emotional situation attached to it that brought up stressful memories. I turned to the next song, “En Mi Viejo San Juan.”
This time, after only a minute, I looked at the monitor. Her blood pressure was now 170. The next piece in the folder was my old standby, “Someone to Watch Over Me.” This time I looked at the monitor in less than 30 seconds. I was stunned. 172. I knew that if it passed 180 she’d be in a hypertensive crisis requiring emergency care. In a critically ill patient that is very serious, and without an intervention, it can be fatal. I remembered an improvisation I’d often used to calm highly agitated patients, a repeating rhythmic pattern that sounded like water flowing in a babbling brook. It had never failed to work. I decided to make one more effort. In the next ten seconds I watched the number climb to 175 and at that moment I was the most scared I’ve ever been in my life. All that went through my mind was: I’m not helping her, this is very serious, I’d better stop and get assistance.
But as I tensed my leg muscles and began to stand I remembered the nurse who’d long ago told me that what she enjoyed most about being a critical care nurse was the detective work. In that moment I thought of Archie Goodwin of the Nero Wolfe crime novels. Archie was Wolfe’s right-hand man. His instructions from Wolfe were that when alone and in a dangerous situation he was to “act in the light of experience as guided by intelligence.”
The brain can make connections, especially in a crisis, at the speed of light. As far as I could tell, I was responsible for this crisis. A split second after thinking of Archie’s instructions, I had a hunch based on experience. I sat down. I would play my hunch but only watch the monitor, not the patient. If it clicked up just one number I’d stop immediately and get Chris or a nurse or doctor as fast as possible. I looked over my shoulder; several staff members were just a few yards away, at another patient’s bed.
The music for the hunch was right on the stand. I started. For about 30 seconds nothing moved. A minute went by. Nothing. Still 175. Then I saw the LED light flicker. The number changed.
175…175…175…174…
About five minutes after I began, Chris and the nurse returned. By then, it was already under 160. I heard Chris say, “Cool,” and leave again. The nurse stayed. I kept going even once the patient had leveled off at 135, playing until I felt it was safe to stop. The first thing I asked the nurse was if they had changed anything while I was playing – medication, anything. She said no. Understanding the reason for my question she said the change in blood pressure was almost certainly caused by the music. Chris came back and checked a few things – the ventilator, the infusion pump, some of the lines – and I asked her the same question. No, she hadn’t changed anything. She looked once more at the monitor, I got a smile and a pat on the back, and she left again. I let out what was probably my all-time personal record for a long sigh of relief.
What was the hunch that I played that had worked so well?
Bach. Of course. But not just any Bach. Fast Bach.
In that moment, when I’d thought of the nurse’s detective remark, I’d remembered two things.
First, I already knew the effectiveness of Bach’s music in post-brain-surgery cases. I was now in my fourth year and had played for dozens of post-brain-surgery patients with complications of some sort, a common occurrence with that kind of surgery but almost always short-lasting. Second, in the year I’d done the Puerto Rican folklore shows with José, I’d played a lot of salsa and merengue music, music with a quick tempo and strong and steady beat, and the audiences loved it. So I combined the two, and it worked. The lingering effect of music, what Dr. McMillen has described as the “blossoming effect,” was the case with the patient in Bed 2. Her blood pressure remained stable for the remaining two days she was in the SICU, a factor in her short stay.
So, the answer to that most often asked question is: you never know. There is no default position. You start out with what you think will be soothing and healing and you go from there, relying on your experience and following any clues you can detect. You act in the light of experience as guided by intelligence. As research psychologist Gary Klein puts it, “Intuition is really a matter of learning how to see – of looking for cues or patterns that ultimately show you what to do.”
Luckily, this story is a one-and-only for me. I have never had such a potentially catastrophic experience before or since. If I had, I would have been long gone from the SICU. For two reasons.
First, the staff, especially the attending physicians, are extremely protective of their patients. If you are not helping, you are gone. Second, my nerves couldn’t take much more of the roller-coaster ride I was on that day. I would have left on my own.
Excerpt from “Waking the Spirit: A Musician’s Journey Healing Body, Mind, and Soul,” by Andrew Schulman. Copyright © 2016 by Andrew Schulman. First hardcover edition published August 2016, by Picador. All rights reserved. Guitarist Andrew Schulman first joined Local 802 in 1975. He has played steady engagements at the Plaza, Mark and InterContinental hotels. Members of Local 802 are welcome to submit personal essays to Allegro for our MEMBER TO MEMBER column. E-mail Allegro@Local802afm.org.
